Hungary has become one of the woeful world leaders in COVID-19 mortality, with overwhelmed hospitals and figures skyrocketing to over 25 daily deaths per million people, compared to over five per million in the EU on average and less than three per million in the USA.
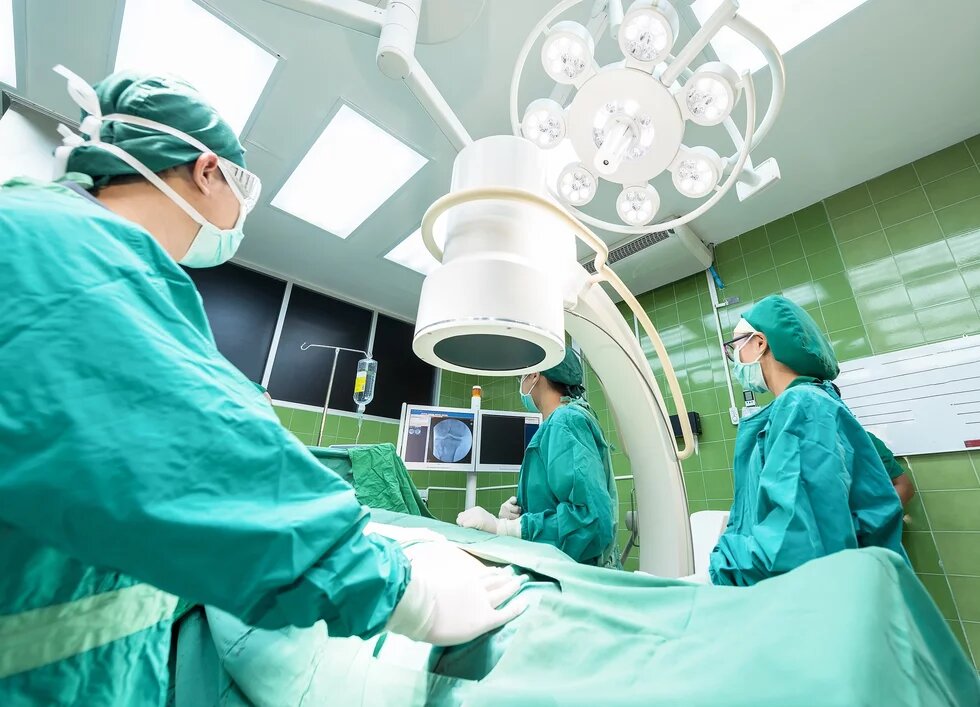
The Hungarian Medical Association has warned of the system becoming saturated despite over 16% of the population having received the first jab and nearly 5% having received the second: “For days we have been world leaders in mortality rates, the majority of hospital units have been turned into COVID-units, the intensive care units are overloaded, the operating theatres have ceased their activity as COVID-patients are now fighting for their lives on operating theatre ventilators. There are no more healthcare workers to be dispatched elsewhere, hospitals are seeking to recruit volunteers.” Also, the president of the Hungarian Ambulance Workers’ Alliance, Zsolt Kusper, told ATV that paramedics have reached the limit of their physical and mental capacities.
Despite this, the new, mandatory contract introduced by Hungary’s government has put further strain on an already-suffering healthcare system. After taking effect on 1 March, the contract, which many public healthcare workers reportedly had to sign on the spot without being consulted ahead of time, has altered their legal status and working conditions. It has created a large pay gap between doctors and other medical personnel; the potential to reduce overtime remuneration for night and weekend shifts; administrative burdens on those who work more than one job – an existential necessity – and technically left them without clarity as to whether they can pursue second jobs at all; criminalized the act of giving or receiving gratuities; and made it possible for workers to be compulsorily detached from their original workplace and reassigned for up to two years.
Fearmongering around the signature
The current increase of doctors’ salaries is a historic achievement that has unfortunately been carried out ingloriously. At certain hospitals, the personnel were obliged to disclose in advance whether they would sign the new contract and told that if they did not sign, they would not find another job elsewhere in the healthcare system, as health expert Dr Zsombor Kunetz describes on his blog. The Trade Union of Hungarian Medical Doctors has also confirmed to the author of this article having received news of such cases of intimidation.
In the end, according to the National Directorate-General for Hospitals, more than 4 000 healthcare workers out of approximately 110 000 in hospitals all over Hungary (doctors, nurses, medical staff) refused to sign the contract and consequently lost their jobs, with many others planning to leave later. One of them is Mónika Töltési, former unit leading chief nurse of the Psychiatry and Addictology Unit of St. Borbála Hospital in Tatabánya. She refused to sign what she calls the “blank contract” of the “slave law” and left public healthcare after a career of 33 years and 10 months. Half of the staff working with her also decided to leave.
Originally the law was supposed to put an end to the long-lasting tradition of patients paying gratuities and to raise the salaries of doctors working in public healthcare, which were comparable to those of fast-food workers. Yet, according to the announcement of the Trade Union of Hungarian Medical Doctors (MOSZ), the law infringes on workers’ right to strike and on the right to bargain collectively. It “contains uncountable controversies, legal insecurities, makes employees vulnerable, entails legal deprivations and restrictions” according to the MOSZ. “Under the Act C. of 2020 on Health Service Legal Relationship [the new healthcare law], healthcare workers' public servant status is terminated, depriving them of the rights and benefits of their legal status as public servants.”
Pay gap creating tension among doctors and medical staff
The Independent Alliance of Healthcare Workers (FESZ) is demanding a comprehensive pay raise for all healthcare professionals and explained to the author of this article that “while doctors will earn 250 – 300% more by the end of the three-step augmentation of their salaries between 2021-2023, nurses, technical health care workers and other medical staff will only have received a salary increase of 72% within 2018-2022. Before, a trained and experienced technical worker with a secondary vocational degree would earn 45-50% of a doctor's wage: This has fallen to 25-30% of a doctor’s wage now. As for nurses with a BSc degree, paramedic officers or midwives with longstanding professional experience, they used to make 75-80% of a doctor's salary, which has now fallen to 40-50% of a doctor’s salary.”
Let us take the example of Mónika Töltési, a chief nurse with 33 years’ work experience and a BSc degree, whose role is to be the glue that keeps a medical team together: If she had signed the contract, she would now earn a gross monthly salary of 1 243 EUR, which means 827 EUR in take-home pay (66.5% of the gross after deductions). A theatre support worker with a secondary school degree and the same work experience would make 771 EUR gross, 531 EUR net: Without these people, operations cannot take place, and all medical examinations that require the patient be moved from one place to another would be blocked. A medical doctor with the same work experience used to make 1 494 EUR gross, 994 EUR net and, according to the first step of the pay raise, will now receive 3 574 EUR gross, 2 377 EUR net. The minimum wage in Hungary is 457 EUR gross, 304 EUR net. The gap between these salaries is frustrating for many.
The timing of the law is very unfortunate: It has created tension between doctors and medical staff and has also caused outrage among doctors over the restrictions introduced. It is happening in the middle of the pandemic’s third wave, in a system that has already been based on the loyalty and self-sacrifice of those who have sworn that they would do everything possible to save patients’ lives.
From the doctors’ perspective, compared to the previous 464 EUR net (which could even be less than the salary of trained nurses or technical assistants with a certain amount of work experience, as certain doctor trainees report), a beginning physician will now earn 875 EUR net, which is a significant change. Doctors in their training years report having earned less in the previous system than a nurse with the added fees of night shifts. In any case, new doctors who have already studied six years to get their medical degrees have had no choice but to sign the contract, as they still have anywhere between three to six years of specialist training ahead of them. On a less positive note, health expert Kunetz, who has criticised the healthcare law for many reasons on his blog, has also pointed out that a packaging worker at ALDI will be earning almost the same as a doctor after 10 years of work.
Petty dealings
What is even less flattering is the way agreements have been reached between employees and hospital directors, Kunetz describes, referring to the example of Ferenc Jahn South-Budapest Hospital, whose director informed the National Public Health Centre on 1 March that the Gastroenterology Unit had become non-functioning because only 20% (i.e., three) of its doctors were ready to sign the new contract. However, shortly after this, it turned out that 12 doctors had finally signed the new contract and that the unit could continue operating. “What was the price paid for this deal?”Kunetz wonders.
The answer he finds is twofold: fearmongering and petty dealings. In the case of this hospital, as Kunetz reports, the director offered special advantages to the doctors of this unit, offering a one-month holiday for March, amidst the raging pandemic, making the treatment of COVID-patients optional for the doctors of this unit, and extremely reducing the number of patients to be treated here for the next three months. Kunetz labels this as extremely unethical, since other units will have to work more as a consequence.
The biggest problem with this law, as Kunetz told the author of this article, is that it conserves the possibility of such petty dealings and secret settlements being made.
Feudalistic system
Mónika Töltési, who still has not received her severance pay following the termination of her employment, says that what made her leave was not the money, but the “contempt” with which medical workers have been treated by their supervisors despite the extreme efforts they made to perform, which have kept increasing throughout the pandemic. The military tone used by the government seems to trickle down through the whole system. Last November, in a reaction to the planned new healthcare law, which contained a list of restrictions and regulations created without any prior debate or consultation with the expert bodies of the profession concerned, the Hungarian Medical Association had already exclaimed that they were not going to be “soldiers”. In his weekly interview on Kossuth rádió on 19 March, Viktor Orbán caused general outrage by calling doctors in their specialist training years “inasok”, which would translate as “servants”, who “have already been dispatched and […] are ready to go when and wherever they need to.”
According to Kunetz, “In the past 10 years, expertise has been exchanged for loyalty in top and middle management. The system lacks creative elements. Nobody dares to take an individual decision, they all await decisions from their superiors, and in the end one person, Viktor Orbán, decides about everything.” Miklós Kásler, Minister of Human Resources, recently appointed new hospital directors to clinical centres, to central hospitals in Budapest and to county hospitals whose mandates began on 1 January 2021. They are the ones who have had to push through the signing of the new contract. While government billboards triumphantly proclaim the historic pay raise for doctors, the situation behind the scenes is rather alarming. Yet, the system still continues to function, as it always has, through the heroic commitment of doctors, nurses and medical workers who will not fail their credo of saving patients’ lives.

